
Book an appointment with one of our expert doctors today,

Treats arterial ulcers by improving circulation and healing wounds through coordinated in-home care.
Learn MoreLearn More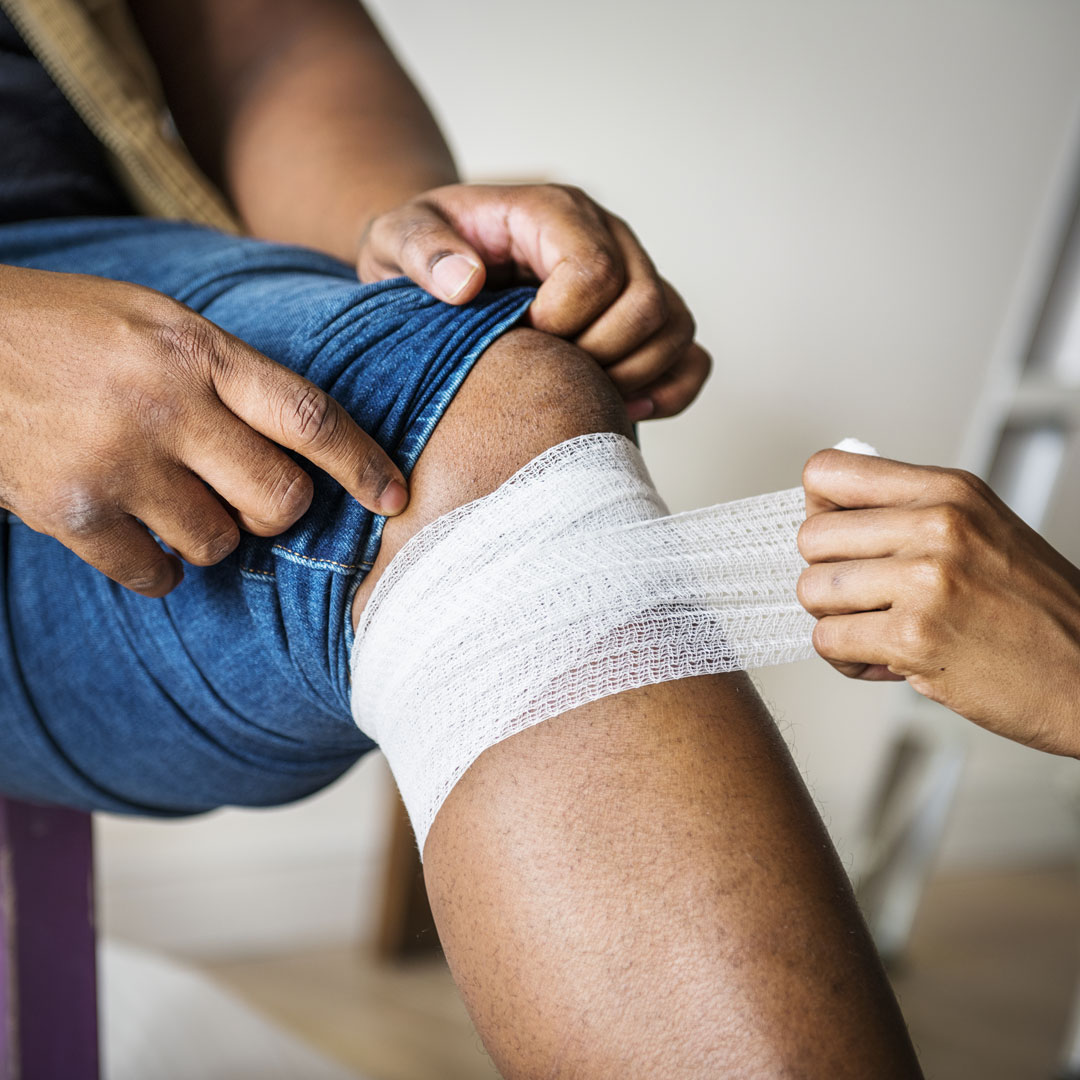
A wound is generally considered chronic when it has not progressed meaningfully through the normal stages
Learn MoreLearn More
In-home care treats diabetic foot ulcers by managing pressure, circulation, infection, and promoting healing.
Learn MoreLearn More
In-home care treats infected wounds with timely intervention, antibiotics, and coordinated physician-led infection management.
Learn MoreLearn More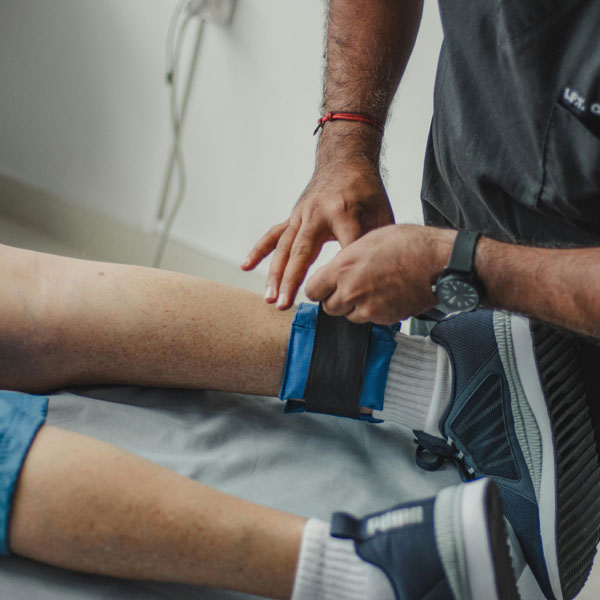
In-home care treats pressure injuries through pressure relief, skin care, nutrition, and effective wound management.
Learn MoreLearn More
In-home care supports surgical wound recovery through monitoring, dressing changes, and coordinated physician-led complication prevention.
Learn MoreLearn More
In-home care treats traumatic wounds quickly, reducing complications and promoting proper healing after injuries.
Learn MoreLearn More
In-home care treats venous leg ulcers using compression, wound care, and lifestyle changes for healing.
Learn MoreLearn More